Understanding Arthritis
What is Arthritis?
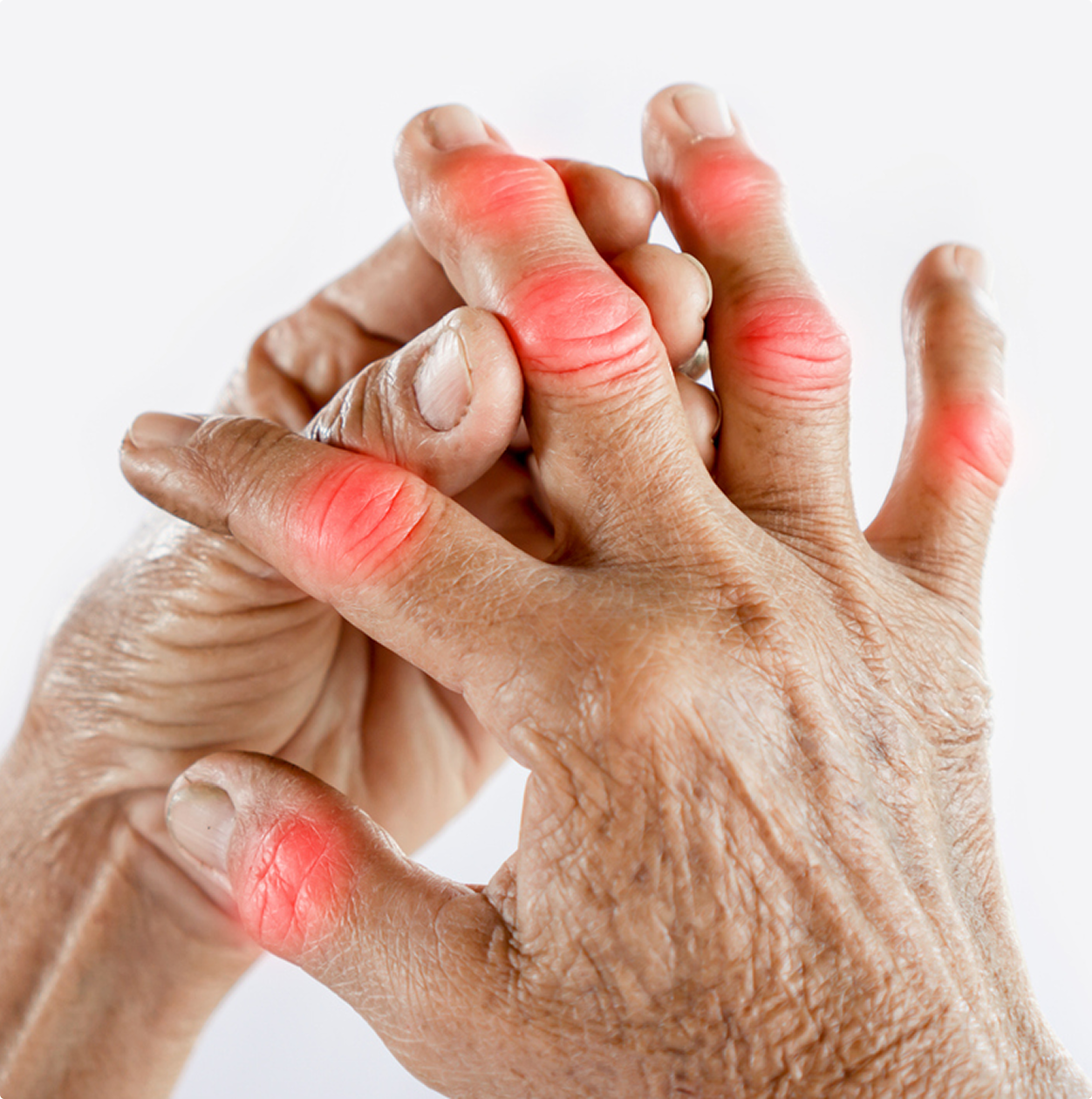
Arthritis is a debilitating disorder that affects millions of people across the country and is one of the leading causes of disability today. In fact, approximately 1 in 5 Americans live with some form of arthritis.
Arthritis is actually not a single disease. Instead, it is an informal way of referring to joint pain or joint diseases. There are over 100 types of arthritis, all with their own symptoms and causes. However, all forms of arthritis can be painful or lead to a loss in quality of life, especially when they aren’t treated properly.