You Are Not Defined By Your MRI Results
Our Bodies Are Resilient, Not Broken
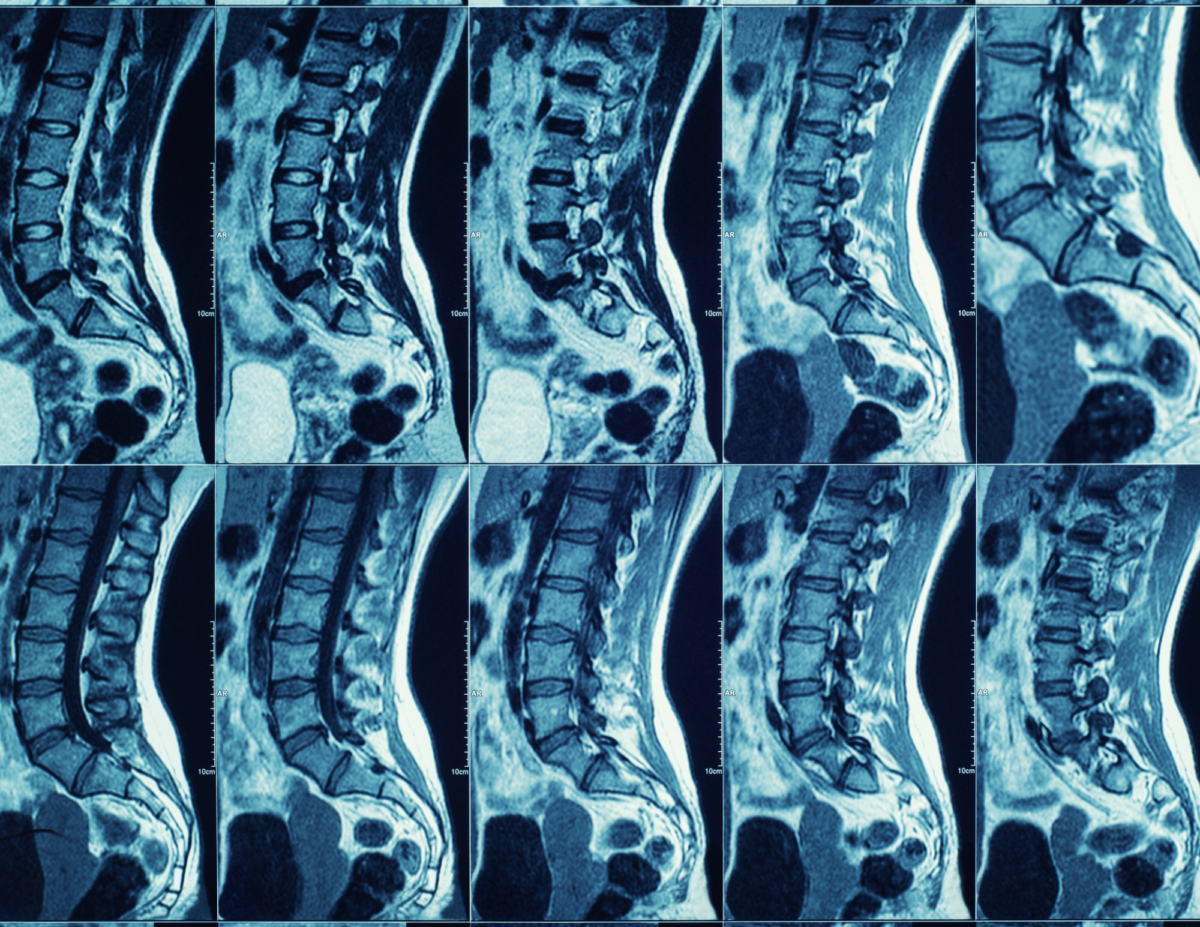
If you have ever received an MRI that showed herniation, degeneration, bone spurs, calcification, or a host of other concerning terms let me assure you that you are NOT broken. While the MRI is a phenomenal invention and can provide life-saving information, it can also cause unnecessary harm and waste billions of healthcare dollars. “Poor” MRI findings cause people to seek unnecessary surgery, take unnecessary medications, and avoid activities they love. Paradoxically, it is the activities they are told not to do (e.g. run, hike, lift weights, play sports) that will reduce pain, improve strength and body resilience, and oftentimes reverse the concerning findings on an MRI.
Our bodies are remarkably adaptive and resilient. They are not broken and in need of “fixing” through surgery and medicine. They often simply need movement.
“Abnormal” Findings Are Normal and Not a Problem
If you receive an MRI on your low back tomorrow, there is a decent chance it will show multiple levels of disc bulges (called herniation), arthritis, decreased space (stenosis), and bone spurs (osteophytes). These “abnormal” findings on an MRI are quite normal. Our bodies degenerate over time; it is a part of life. Most patients with symptoms have normal MRI reports while a significant portion of patients without symptoms (asymptomatic) have “abnormal reports.” This is not exclusive to the low back. Imaging studies on the neck, shoulder, hip, ankle, knee and show similar findings. MRIs routinely show degeneration of cartilage in the knee, hips, and ankles or runners, yet they are pain free.
Psychosocial factors, including anxiety, depression, attitudes and beliefs, social context, or work status may all play an important role in the pain experience. We don’t simply have ‘pain fibers’ that are turned on and off. While we do have nociceptors, which have often been misclassified as ‘pain fibers’, they are influenced by many psychosocial influences and are not the only source of a pain stimulus. Degeneration occurs with aging and often the findings on an MRI do not need to be addressed with external means (medication, injections, surgery). Instead, allow your body to improve through exercise. The hyperfocus on the findings are often what worsens the pain.
When Are MRI’s Useful?
Receiving an MRI is oftentimes more harmful than beneficial. Receiving an MRI as a first-line assessment can lead to poorer outcomes for patients with low back pain. The MRI causes fear-avoidance behaviors as patients are scared to move, fearing movement will cause further “damage”. In reality, lack of movement often intensifies symptoms and delays recovery. Advanced imaging adds anywhere from roughly $2,500 to $4,800 in additional costs to the total bill for treating back or neck pain. These costs come through unnecessary additional tests, medication prescription, injections, delayed physical therapy, lost time at work, and surgery. If instead, the first-line approach was to encourage movement, unnecessary treatments (medication and surgery) could be avoided.
MRIs are not very helpful, except in the case of serious medical pathology, such as finding a tumor. I do not want you to think tissue damage is irrelevant. If you cut your finger or tear a muscle, you will more than likely feel pain and the injury will take time to recover. That recovery however will occur naturally with a gradual increase in activity. Furthermore, the damage is only a small piece of the pain puzzle.
If MRI’s Don’t Explain Pain, What Does?
Our emotional status and history of pain can significantly impact our pain experiences as well. This is a primary reason why chronic pain is so prevalent and difficult to treat. When we experience pain for a prolonged period — that is, beyond the duration of normal healing — our nervous system is hypersensitive. Other stressors such as poor or insufficient sleep, poor dietary habits, inactivity, other medical conditions, and…well, stress (for example, racking up six-figures of debt for school, living with kids who think sleep is optional, being a Miami Dolphins fan, and other completely random things I know nothing about), can lead to a heightened pain response. This causes traditional treatment approaches — such as surgery and medication — to be ineffective as they fail to treat the nervous system and the multiple factors contributing to the pain.
What does this mean for you? The next time your doctor prescribes an MRI, ask why you need it. If there are no signs of serious pathology, such as cancer, then an MRI is not needed. Instead, consult with your local physical therapist to develop a comprehensive, personalized treatment plan that encourages movement and helps you achieve your desired goals.
ABOUT THE AUTHOR

Zach Walston (PT, DPT, OCS) grew up in Northern Virginia and earned his Bachelor of Science in Human Nutrition, Foods, and Exercise at Virginia Polytechnic Institute and State University. He then received his Doctorate of Physical Therapy from Emory University before graduating from the PT Solutions’ Orthopaedic Residency Program in 2015.
Zach has numerous research publications in peer-reviewed rehabilitation and medical journals. He has developed and taught weekend continuing education courses in the areas of plan of care development, exercise prescription, pain science, and nutrition. He has presented full education sessions at APTA NEXT conference and ACRM, PTAG, and FOTO annual conferences multiple platforms sessions and posters at CSM.
Zach is an active member of the Orthopedic and Research sections of the American Physical Therapy Association and the Physical Therapy Association of Georgia. He currently serves on the APTA Science and Practice Affairs Committee and the PTAG Barney Poole Leadership Academy.