Patellofemoral Pain Syndrome: A Case Series
Patellofemoral Pain Syndrome: A Case Series
Erin Golden, PT, DPT
STUDY DESIGN: Case Series BACKGROUND: There is no gold standard treatment for patients with patellofemoral pain syndrome. The purpose of this case series is to show whether hip strengthening with spinal manipulation helps decrease pain and improve the athletes’ function. CASE DESCRIPTION: The three patients were all athletic females, ages 15-16, who suffer from patellofemoral pain syndrome. OUTCOMES: All three female athletes did report feeling stronger while performing their activity. In the eight weeks of treatment, one of the patients was still experiencing pain at times but had reported a decrease in severity of pain. All three patients made significant improvements with all functional outcomes. DISCUSSION: Patellofemoral pain syndrome is known to be a multifactorial problem. However, further research needs to be performed to determine which treatment techniques are most effective at decreasing pain and improving function. LEVEL OF EVIDENCE: Level 4 KEY WORDS: Patellofemoral pain syndrome, hip strengthening, spinal manipulation
INTRODUCTION
Patellofemoral pain syndrome (PFPS) is a common diagnosis seen in athletic individuals that can be burdensome to their ability to participate in their activity of choice. Younger individuals, ages 15-30 years, tend to be diagnosed more so than the older population, and it is estimated that 25-40% of all athletes with complaints of knee pain have PFPS.2,4 Females specifically have a higher incidence of developing.4 It has been shown in the literature that this is a multifactorial problem, and there is evidence that proximal and distal strength deficits possibly lead to PFPS.10,19 With this being said, it can be a difficult and frustrating diagnosis to treat on both ends of the spectrum, especially when the athlete continues to participate in their sport.6 There is a very high reoccurrence of pain and many athletes tend to reduce their activity level because of pain. It is estimated that 70-90% of individuals have recurrent or chronic patellofemoral pain.18 Therefore, physical therapists must truly refine the proper way to treat patellofemoral pain in order to give patients the most optimal outcome.
The patella does not just move superior and inferior; it also tilts and rotates. All of these motions can be affected causing an increase in pain. Many anatomical or physiological issues can lead to patellofemoral pain, including improper patellar tracking, weakness of musculature, tight musculature surrounding the knee, and pes planus deformity.14 Because patellofemoral pain is a multifactorial problem, there have been many studies assessing various interventions to help decrease pain and improve function. Quadriceps strengthening (VMO strengthening specifically), gluteal/hip strengthening, patellar taping, bracing, foot orthotics, and spinal manipulation have all been assessed to determine the efficacy of this treatment.1,2,3,7,9,13,16 It has been shown effective to treat athletes using more than one of these interventions2, but it is not known which exercises are most effective at improving strength and improving lumbopelvic mechanics in order to improve their tolerance for activities. Some patients even resort to surgery to correct for this problem, but exercise has actually been shown in the literature to be as effective.15 If this is the case, physical therapy is obviously the most cost effective means of treatment. Physical therapists need to further investigate which interventions will be most effective.
Earlier studies examining strengthening have focused specifically on quadriceps or VMO, but more recent studies have assessed the outcomes of performing hip strengthening solely to determine if quadriceps strengthening is as significant as previously thought.1,3 In addition to hip strengthening, it is important to determine whether closed chain or open chain exercises are most effective.8 Evidential support in the literature exists for both, 5,11,22 but knowing which specific exercises are most effective for the patient with patellofemoral pain syndrome is vital.
There is growing evidence to support hip strengthening specifically1, but little evidence exists that combines hip strengthening with spinal manipulation to treat patellofemoral pain syndrome.12 We already know that altered lumbopelvic mechanics can cause added stress at the knee, hence it would benefit physical therapists to evaluate corrected faulty mechanics in the treatment of PFPS. The purpose of this case series is to describe the effectiveness of hip strengthening with spinal manipulation.
CASE DESCRIPTION
Subjects
Three female athletes, ages 15-16 year of age, were included in this study. All came to therapy with complaints of anterior knee pain. Inclusion criteria for this case series involved being female, participating in a sport for at least six months during the year, being 14-18 years of age, and experiencing pain in anterior knee with squatting, ascending/descending stairs, and dynamic landing activities. Exclusion criteria for this study included prior history of knee surgery, concurrent treatment by another health care professional for same diagnosis, positive tests for ligamentous or meniscal injuries, and refusal to fully participate in exercises or spinal manipulation.
Patient 1 is a 15-year-old female with a history of left anterior knee pain intermittently for over a year. She is a competitive cheerleader who practices over 15 hours per week, performing high dynamic landing activities. She initially began noticing a gradual increase in pain while participating in competitive cheerleading which progressed to pain with all weight bearing activities, specifically squatting or stair activities. She had been in physical therapy for two months without improvement that ended about six months prior to this episode of care. That bout of physical therapy focused on global lumbopelvic, hip, and lower extremity strengthening which had not been helping alleviate pain during activities. Upon beginning the current session of physical therapy, she had been resting from cheerleading for six months. She had begun to return to sport one month prior to beginning this study. She had mild complaints of pain, only occasionally before beginning this treatment, but patient and family wanted to return to therapy again to improve strength and mechanics, so her symptoms did not progress, resulting in a cessation of cheer.
Patient 2 is a 15-year-old female, who also is a competitive cheerleader, with complaints of left anterior knee pain. She has been experiencing pain intermittently for two years. During off-season, she practices at least six hours per week, and during season she practices at least 14 hours per week. At the time of this study, she was practicing at least six hours each week. She noticed an increase in pain not only with cheering, but also with prolonged sitting, squatting, and stairs. She had never received physical therapy but had self-treated with rest, ice, medication, and bracing, which only relieved pain temporarily.
Patient 3 is a 16-year-old female softball player who had been experiencing pain in left knee for almost a year. She noticed an increase in pain while playing softball and with squatting, kneeling, and prolonged sitting. She had never received any treatments from healthcare professionals prior to this case series and had been managing independently with ice and stretches, which yielded no results.
Outcome Measures
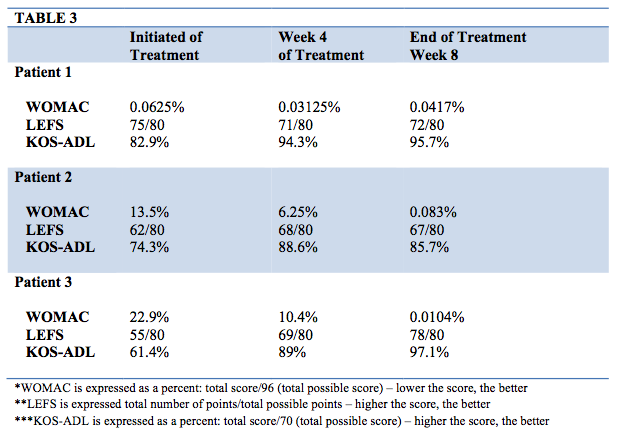
The outcome measures utilized in this study were the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Lower Extremity Functional Scale (LEFS), and the Knee Outcome Study – Activity of Daily Living (KOS-ADL). The WOMAC assesses pain, stiffness, and physical function and is typically used to assess knee osteoarthritis, but can also be utilized to assess pain and function related to patellofemoral pain. The LEFS is commonly used to assess the level of difficulty with functional activities and is recommended as a functional outcome with PFPS. 20 Lastly, the KOS-ADL assesses the symptoms and limitations experienced due to knee pain. All three have been shown to be reliable and responsive to change.21 Questionnaires were completed at beginning, after four weeks, and at the end of the eight weeks of treatment.
Intervention
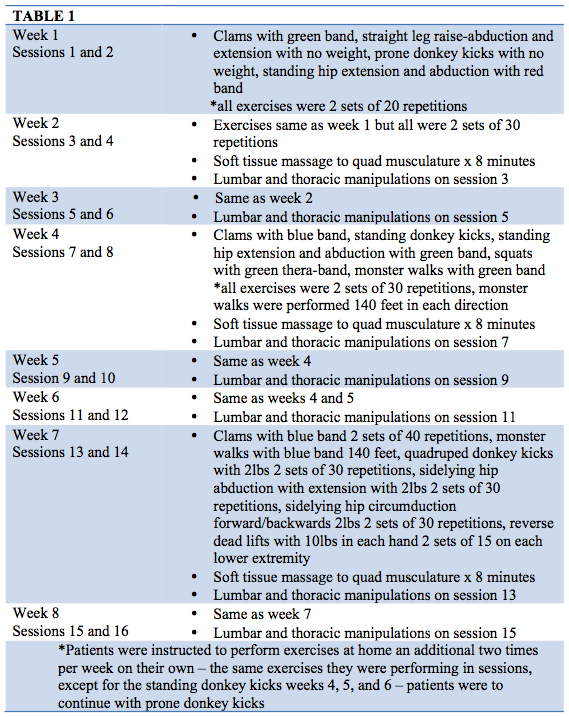
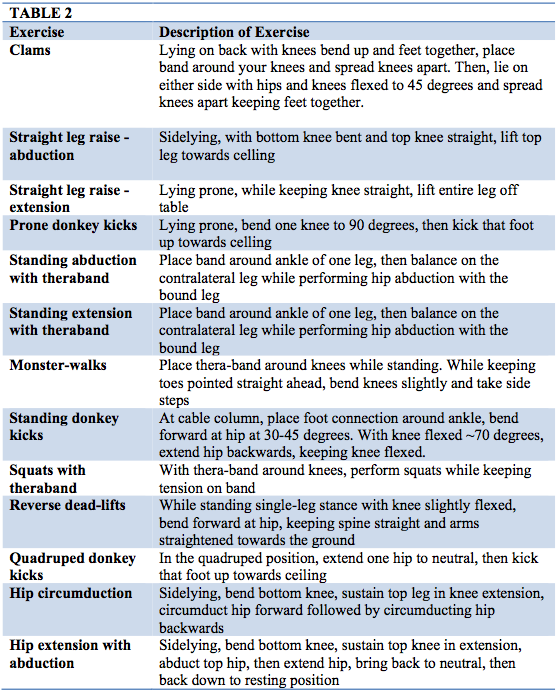
All three patients received the same interventions when they attended therapy sessions. They each performed the same exercises using the same resistance theraband and performed the same number of repetitions. Each patient also received soft tissue to the quadriceps musculature and thoracic and lumbar manipulations. See Table 1 for interventions received each week. Table 2 describes the exercises being performed. Patient 1 did receive soft tissue work to her affected calf musculature as well as dry needling in weeks 3-5, since she was experiencing tightness and feelings of a “Charlie horse” with activity. Patient 2 received patellar taping once per week, for the first three weeks of treatment, to better control her pain level and improve her tolerance for cheerleading activities.

OUTCOMES
All patients began to report feeling stronger while performing their specific sport. One of the three females, Patient 2, still reported experiencing some pain at the end of the eight weeks of treatment but did report the severity of pain decreasing. All three patients made significant improvements with functional outcomes. See Table 3 for functional outcome data.
DISCUSSION
Patellofemoral pain syndrome can cause high-level athletes to miss out on their sporting activities because healthcare professionals do not know exactly how to treat the pain. Ample literature exists on various aspects of treatment, yet there is still no gold standard of treatment.
Literature has shown repetitively that strengthening alone results in increased tolerance for functional activities after therapy. There is support for quadriceps and hip strengthening both independently and in combination. Home exercise programs are imperative for patients. Many high-level high school athletes are busy with their school schedules, and when combined with sport for 15-20 hours per week, time runs short for home exercises. The most effective interventions must be determined to help facilitate athletes’ to return to sport.
All three patients showed progress during the eight week treatment of utilizing hip strengthening, soft tissue work to quads, and thoracic/lumbar manipulations. However, further questions do need to be answered: Is eight weeks truly long enough to show changes? At what frequency and duration should patients be treated? Is our best form of treatment combining multiple approaches of interventions?17 Future studies, such as randomized controlled, are needed.
CONCLUSION
There is no gold standard for treating patellofemoral pain syndrome. The three females in this study showcased signs of improvement following hip strengthening and lumbar manipulation over an eight week period, but two still had some pain and difficulty with their sport. Although strengthening, patellar taping, and foot orthotics have all been effective, future studies, in the form of randomized controlled trials should assess whether combination of treatments are necessary in treating PFPS.
- Barton, CJ, Lack, S, Malliaras, P, Morrissey, D. Gluteal muscle activity and patellofemoral pain syndrome: a systematic review. Br J Sports Med. 2013; 47:207-214.
- Bizzini M, Childs JD, Piva SR, Delitto A. Systematic review of the quality of randomized controlled trials for patellofemoral pain syndrome. J Orthop Sports Phys Ther. 2003;33:4-20.
- Bolgla, LA, Malone, TR, Umberger, BR, Uhl TL. Comparison of hip and knee strength and neuromusculature activity in subjects with and without patellofemoral pain syndrome. Int J Sports Phys Ther. 2011; 6(4):285-96.
- Boling M, Padua D, Marshall S, Guskiewicz K, Pyne S, Beutler A. Gender differences in the incidence and prevalence of patellofemoral pain syndrome. Scand J Med Sci Sports 2010; 20(5): 725-30.
- Boling, MC, Bolgla, LA, Mattacola, CG, Uhl, TL, Hosey, RG. Outcomes of a weight-bearing program for patients diagnosed with patellofemoral pain syndrome. Arch Phys Med Rehabil. 2006; 87:1428-35.
- Collado, H, Fredericson, M. Patellofemoral pain syndrome. Clinics in Sports Medicine. 2010; 29(3):379-98.
- Eng, JJ, Pierrynowski, MR. Evaluation of soft foot orthotics in the treatment of patellofemoral pain syndrome. Phys Ther. 1993: 73(2):62-68.
- Fagan, V, Delahunt, E. Patellofemoral pain syndrome: a review on associated neuromuscular deficits and current treatment options. Br J Sports Med. 2008; 42:789-95.
- Gross, MT, Foxworth, JL. The role of foot orthoses as an intervention for patellofemoral pain. J Orthop Sports Phys Ther. 2003; 33:661-70.
- Fredericson M, Yoon K. Physical examination and patellofemoral pain syndrome. Am J Phys Med Rehabil. 2006;85:234-243.
- Herrington L, Al-Sherhi A. A controlled trial of weight-bearing versus non-weight-bearing exercises for patellofemoral pain. J Orthop Sports Phys Ther. 2007; 37:155-160.
- Iverson CA, Sutlive TG, Crowell MS, Morrell, RL, Perkins, MW, Garber MB, Moor JH, Wainner, RS. Lumbopelvic manipulation for the treatment of patients with patellofemoral pain syndrome: development of a clinical prediction rule. J Orthop Sports Phys Ther. 2008; 38:297-309; discussion 309-212.
- Johnston LB, Gross MT. Effects of foot orthoses on quality of life for individuals with patellofemoral pain syndrome. J Orthop Sports Phys Ther. 2004;34:440-448.
- Juhn, M. Patellofemoral pain syndrome: a review and guidelines for treatment. Am Fam Physician. 1999; 60(7):2012-18.
- Kettunen, JA, Harilainen, A, Sandelin, J, Schlenzka, D, Hietaniemi, K, Seitsalo, S, Malmivaara, A, Kujala, U. Knee arthroscopy and exercise versus exercise only for chronic patellofemoral pain syndrome: 5-year follow-up. Br J Sports Med. 2012; 46:243-46.
- Lesher JD, Sutlive TG, Miller GA, Chine NJ, Garber, MB, Wainner, RS. Development of a clinical prediction rule for classifying patients with patellofemoral pain syndrome who respond to patellar taping. J Orthop Sports Phys Ther. 2006;36:854-866.
- Lowry, CD, Cleland, JA, Dyke, K. Management of patients with patellofemoral pain syndrome using a multimodal approach: a case series. J Orthop Sports Phys Ther. 2008; 38(11): 691-702.
- Powers CM, Bolgla L, Callaghan M, Collins, N, Sheehan F. Patellofemoral pain: proximal, distal, and local factors 2nd international research retreat. J Orthop Sports Phys Ther. 2012; 42 (6):A1-A20.
- Reiman, MP, Bolgla, LA, Lorenz, D. Hip function’s influence on knee dysfunction: a proximal link to a distal problem. J Sport Rehabil. 2009; 18:33-46.
- Watson, CJ, Propps, M, Ratner, J, Zeigler, DL, Horton, P, Smith, SS. Reliability and responsiveness of the lower extremity functional scale and the anterior knee pain scale in patients with anterior knee pain. J Orthop Sports Phys Ther. 2005; 35(3):136-46.
- Williams, VJ, Piva SR, Irrgang, JJ, Crossley, C, Ftizgerald, GK. Comparison of reliability and responsiveness of patient-reported clinical outcome measures in knee osteoarthritis rehabilitation. J Orthop Sports Phys Ther. 2012; 42(8):716-23.
- Witvrouw, E, Lysens, R, Bellemans, J, Peers, K, Vanderstraeten, G. Open versus closed kinetic chain exercise for patellofemoral pain: a prospective, randomized study. Am J Sports Med. 2000; 28(5):687-94.